An unparalleled and focused array of extensively-tested biomarkers that have been shown to highly correlate with age.
Heart disease affects more people than any other disease or illness, and can develop without any symptoms. Some people may not be aware of heart disease until they have a heart attack, stroke or other health problem.
Traditionally, cardiovascular age has been measured by the change in blood pressure. More informative and precise techniques have been developed to measure this change in stiffness of arteries as they age. At PhysioAge, we use cutting-edge technology to provide a detailed analysis of your heart health.
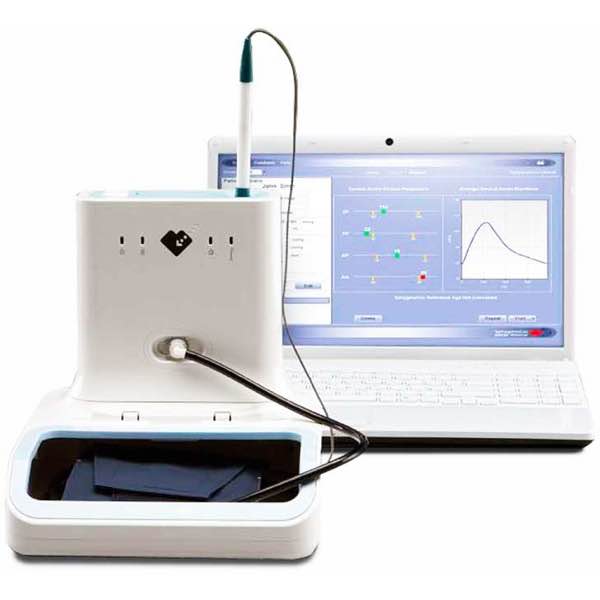
SphygmoCor is an FDA-approved device that is becoming the gold standard in trials that assess the effectiveness of blood pressure medications and can now be found in a few doctors’ offices around the globe. We perform this measurement on all patients to measure their baseline vascular age and to see how our programs are affecting it.
Blood pressure Pulse Wave Analysis is new technology that assists your doctor in assessing your arterial and cardiovascular health. Blood pressure measured in your arm is not the same as the blood pressure at your heart. It is your blood pressure at your heart that affects the performance of your heart, and pulse wave analysis determines your blood pressure at your heart and gives your doctor valuable information about the interaction between your heart and blood vessels. This new technique therefore complements the conventional blood pressure cuff and provides additional information on cardiac function. The test is simple and painless, taking only a few minutes to perform using a sophisticated blood pressure cuff on your arm. Then the Pulse Wave Analysis system will calculate the pressure waveform at the heart and provide your physician with cardiovascular measurements such as Alx, ED and SEVR.
Augmentation Index is a measure of the stiffness of your arteries. High cholesterol, smoking, diabetes, and aging can all cause the vessels that take blood from the heart (the arteries) to become stiffer. As the arteries become stiffer the heart must work harder due to the extra load on the heart.
Each time our heart beats, it has a time when it is contracting and pumping blood out of the heart, and a time when it is resting and filling with blood. The ED is a measurement of how much time the heart spends pumping. When the heart spends a shorter time than normal pumping there may be problems with the ability to pump blood, while longer than normal pumping time may indicate problems with the ability for the heart to relax and fill with blood.
When the heart is resting, the heart muscle is supplied with oxygen for energy. When the heart is contracting and pumping this energy is being used. The SEVR is a measure of the ability of the arterial system to meet the heart’s energy requirements. As this ratio decreases, the heart has less energy reserves available and may have a lower tolerance for physical activity.
Heart disease can be treated using a combination of diet, exercise and drug therapies. Your doctor will use this information to assist with making decisions on whether you need treatment, and if so what treatment options are best for you. It is important for your physician to see how your cardiovascular assessment changes in response to treatment. For more information on wave reflection, visit Atcor Medical’s excellent tutorial presentation and flash animation.

You may be wondering, “Why do I need a fancy instrument to tell me how well my skin is aging.” Most of think that just looking in the mirror ought to suffice, yet studies have demonstrated that facial skin appearance (photoaging) is more affected by the amount of sun exposure than chronological age. As such it is not a great biomarker of aging. Interestingly, intrinsic skin aging, the loss of elasticity and fine wrinkling that occur in areas of your body that receive relatively little sunshine, correlates very closely with age. Even more interesting, is that the linear change in elasticity is hard to appreciate with the naked eye until it is relatively advanced.
To measure intrinsic skin aging we use the Cutometer, an instrument that has been validated in hundreds of studies of skin aging over the past 25 years. It works by applying a sequence of precise and gentle suctions to a small area of skin and then measuring with an optical sensor how much the top two layers of your skin move with each suction. The movement is very slight—only 0.2-0.5 mm—much less than the amount it moves when doing a “pinch test” to see how fast your skin returns to normal after pinching it between your two fingers, pulling it up, and releasing it. Yet by involving only the top two layers, the Cutometer can non-invasively assess the amount and structure of the collagen and elastic in your skin. The result is reported as skin elasticity percent: the extent to which your skin returns to its original position after being stretched and released. When you finish adolescence, the average skin elasticity is almost 90%; with each passing year the average person loses about 1%, leaving the average 80 year old with about 35% elasticity.
Skin elasticity as measured by the Cutometer has been correlated with bone density and shown to be improved by HRT in women. For many years elasticity measurements with the Cutometer® have been recognized as the gold standard in dermatology and cosmetology and have been used to support the latest discoveries in both fields. Due to its precision and ease of use compared to other elasticity measurement methods, the Cutometer® is mentioned in most studies on this subject worldwide.

Most of us are familiar with the “breathing tests” that asthmatics and emphysema patients take to see how their disease is fairing either during a flare up or routine monitoring of the their medications—inhalers and such. Yet if you don’t have any lung disease, you are unlikely ever to have taken such a test. We, and many prominent pulmonary specialists, think that is unfortunate.
Spirometry, as the breathing test is called, turns out to be a interesting biomarker of aging hiding in the clothing of pulmonary specialist’s test. While it certainly functions as a screen for early lung disease in undiagnosed asthmatics and smokers, it also measures the lung age of healthy individuals. In fact, in order to determine if the result of a spirometry test is abnormal, it must be compared to a large database of normal results adjusted for height, gender, ethnicity, and age. Spirometry performed by tens of thousands of individuals has resulted in large databases which can be used to determine lung age.
The complete testing session takes about 10 minutes. The patient takes as deep a breath as possible, places the airflow meter (pneumotach) in his mouth, then blows out the air as fast as possible in the first second. He then continues to blow for at least 5 seconds longer in an effort to completely empty his lungs. The computer attached to the pneumotach calculates the total amount of air expelled during the full exhalation, and the amount expelled in the first second. These measures are called the forced vital capacity (FVC), and the forced expiratory volume in the first second (FEV1), respectively. The procedure is repeated until 3 consistent measures are recorded.
Both the FVC and FEV1 decline after about age 25, but the FEV1 is the best marker. It declines about 1 to 2 percent per year as the graphs below depict.
Many people are afraid to take a cognitive test because they think they will “fail it.” This is unfortunate because they are no more likely to “fail it” than they are the tests of lung and arterial function. It’s like thinking that because you get a little shorter of breath running up a flight of stairs now than when you were younger, you are going to get lung cancer or have a heart attack.
As early as your mid-twenties, certain aspects of your cognitive function begin to decline in a linear fashion. You don’t notice the decline unless you tax the system, e.g., play a video game or do long division in your head. If that decline is steeper than the average person, you are more likely to have significant neurologic disease decades later than someone whose decline is average, and now is the time to act.
The CNS Vital Signs battery of neuropsychological tests assesses the main areas of cognitive function, by taxing them more than your daily activities (Most people find the 20-minute battery to be quite challenging). It is used to screen for significant neurologic impairment from dementia, ADHD, or medications and is a screening test that everyone should take periodically. Just as we saw with spirometry, however, in order to know if there is a significant impairment, the results of the test must be age-adjusted. While most domains of cognitive function are affected by normal brain aging, two areas are particularly sensitive to age and start early in adulthood.
These domains of cognitive function are called ‘reaction time,’ ‘psychomotor speed,’ and ‘processing speed.’ The Stroop Test measures how quickly and accurately you can apply a rule to a stimulus and then inhibit the application of that rule (first act when the word spells the color of its font/then reverse the rule). The Symbol Digit Coding test measures how many paired sets of symbols and digits you can process on a computer screen with your eyes and then press the corresponding key on the keyboard. Cognitive neuroscientists have shown that the decrease in performance on tests like these is correlated with the loss of dopamine activity in the frontal lobes of the brain.
Your NeuroAge is a weighted composite of the scores on these two tests.
Not surprisingly, as we age, our immune systems falter. Older adults are more likely to succumb to infections their younger selves blithely warded off with barely a sniffle. Cancer rates increase exponentially with age, partly because of less effective tumor surveillance from an aging immune system. Dysfunctional immune cells cause chronic inflammation which increases the likelihood of degenerative diseases such as osteoporosis, atherosclerosis, and dementia. This condition, called ‘immunosenescence,’ results from changes in the relative proportions and function of subsets of white blood cells, the thymus, and the bone marrow.
One of the most prominent changes of immunosenescence is the decrease in the subset of white blood cells that are able to fight off new infections or tumors. Called naïve suppressor t-cells, they are designated by the lack of the CD95 and presence of the CD28 molecules protruding from the membranes of the cell’s surface. The presence of these CD95-CD28+ t-cells can be detected at specialized labs from the same of tube of blood used to do the routine CBC (complete blood count). Cells that do not have CD95 sticking out of them have not yet encountered the foreign substance (the molecular snippet of an infectious bug or tumor), called ‘antigen,’ they are uniquely created to recognize. The CD28 molecule enables these cells to divide rapidly and mount a brisk response to their designated antigen, which results in clearance of the infection/tumor.
The linear decline in the number of CD95-CD28+ t-cells is so highly correlated with age (r2 >0.5) that it has been called the best biomarker of immune aging discovered to date. When we are young adults, we have over 200-250 cells/mcl of blood but start to lose about 3 cell/mcl per year from then on. If you do the math, you can see that this leads to complete absence of the ability to fight off new infections and tumors by the ninth decade, which is just about the average life expectancy. If you add B-lymphocytes (CD19+) to the model with naïve t-cells, your understanding of age-related immune system changes increases even more (r2 >0.63).
If there is a candidate to be considered the human body’s molecular clock, then one of the front runners must certainly be the length of our telomeres. From the Greek, telos, meaning ‘end,’ and mere, meaning ‘part,’ telomeres are the caps on the ends of each of our chromosomes that protect them from being mistaken for damaged DNA. They are composed of thousands of repetitions of the same sequence of 6 base pairs (the letters of DNA), TTAGGG. With each cell division, they shorten by about 50-100 base pairs because of the difficulty DNA polymerase has replicating one of the strands. At young adulthood, the mean lymphocyte telomere length (MTL) is about 8 kb (8,000 kilo base pairs). Once it reaches 4 kb, the cell no longer is able to divide and enters what is called ‘replicative senescence,’ in which it fails to perform its function and produces detrimental inflammatory molecules. The molecular clock stops ticking.
The subset of your white blood cells used to calculate your ImmunoAge, the lymphocytes, is the cell type whose telomere length has been most studied. This is mostly because of its easy access through a routine blood draw, in contrast to a biopsy of, for example, your lungs or arteries. Hundreds of studies have linked the shortening of lymphocyte MTL not only to the aging process, but also to cardiovascular disease, smoking, various cancers, and even psychological stress. (A few studies have measured the correlations between MTL and the telomere lengths of other tissues in the body and have found general agreement.)
The average person’s lymphocyte MTL decreases about 30-50 base pairs per year; you are more likely to be in the higher end of this range if you smoke, don’t exercise, have a lot of stress, or have a chronic disease. Thus, if you start out with a lymphocyte MTL of 8 kb and lose 0.04 kb/yr (40 base pairs), you will get to the critical length of 4 kb in 66 years, again, very close to the average human lifespan. The correlation with age for this biomarker is in the range of an r2 of 0.5.
You may be thinking, “If you telomere length functions as such a great biomarker of aging and disease, why don’t we just measure it instead of bothering with all these other tests?” We wondered about that too as we were searching for the best biomarkers of aging. To our amazement, we found that while telomere length correlates with age very well, the combination of biomarkers including it correlate much better—r2 0.8 versus 0.5—confirming the notion that the aging process is best understood by looking at combinations of biomarkers of important physiological systems.
Medical and statistical significance
Our expert system is based on solid science – extensive clinical trials, scientific literature, and careful statistical analysis of primary data. Rather than using secondary clinical studies to calculate physiological age, we used our own in-depth primary research to measure up to 120 attributes in a database of 4,500 individuals. This study determined how biomarkers relate to each other, which enabled a greater degree of statistical accuracy and a deeper understanding of the aging process. With unique in-house measurements, PhysioAge® gives you complete, clear, and precise results.
Edmonds Wellness Clinic
7935 216th St. SW, Suite E
Edmonds, WA 98026
Phone:
(425) 672-2113
Get Directions
We work with a wide range of insurance providers and also offer self-pay options.